

Symptoms
- Pelvic pain generally refers to burning, itching, aching or other types of pain in the vulva, vagina, perineal, and/or anal area
- Women with pelvic pain often suffer from pain with intercourse, may experience hypersensitivity when wearing pants and/or underwear, and may have pain with sitting
- Exercise may provoke or exacerbate symptoms
- In addition to pelvic pain, women can also experience urinary urgency, frequency, pain with urinating, and/or urinary leakage
- Women may suffer from abdominal bloating, gastrointestinal distress, and constipation
- Symptoms can be provoked, meaning with penetrative intercourse or tampon insertion, or unprovoked and spontaneous
- Symptoms can be intermittent or constant

Symptoms
- Pelvic pain generally refers to burning, itching, aching or other types of pain in the vulva, vagina, perineal, and/or anal area
- Women with pelvic pain often suffer from pain with intercourse, may experience hypersensitivity when wearing pants and/or underwear, and may have pain with sitting
- Exercise may provoke or exacerbate symptoms
- In addition to pelvic pain, women can also experience urinary urgency, frequency, pain with urinating, and/or urinary leakage
- Women may suffer from abdominal bloating, gastrointestinal distress, and constipation
- Symptoms can be provoked, meaning with penetrative intercourse or tampon insertion, or unprovoked and spontaneous
- Symptoms can be intermittent or constant
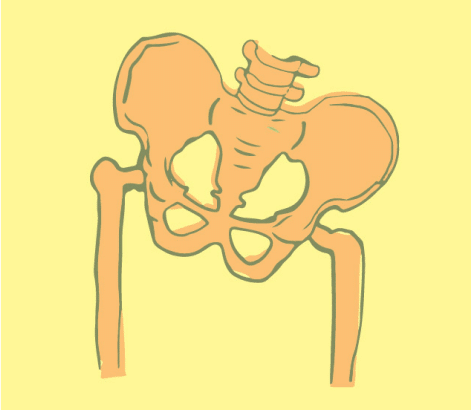
Associated Diagnoses
Diagnoses such as Endometriosis, Vulvodynia, Interstitial Cystitis/Painful Bladder Syndrome, Pudendal Neuralgia, Lichen Sclerosus, Lichen Planus, and Irritable Bowel Syndrome are associated with pelvic pain and pelvic floor dysfunction.
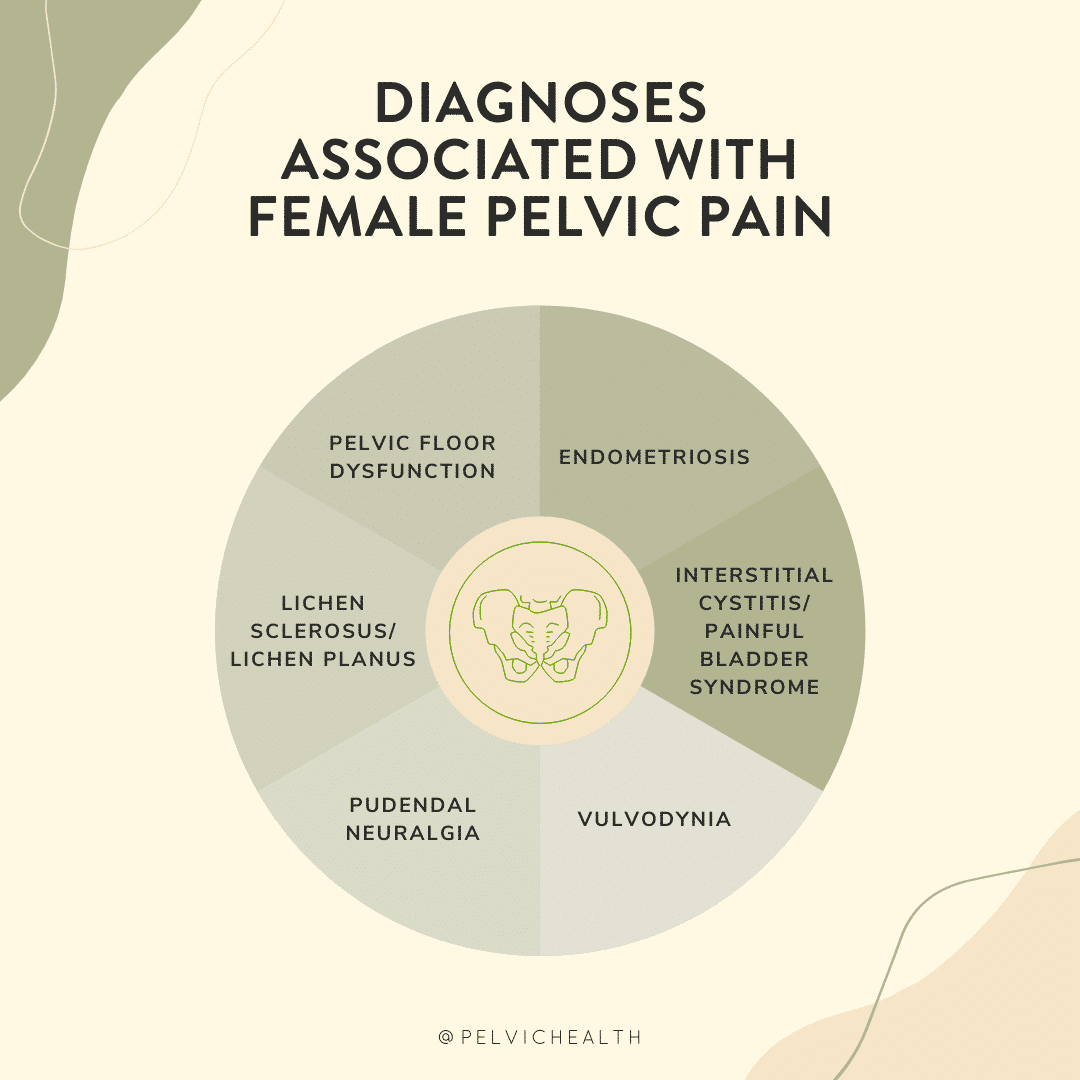
Causes of Pelvic Pain
- Repetitive vaginal and/or bladder infections and/or gynecologic, urologic, dermatologic or gastrointestinal conditions
- The majority of women with pelvic pain have pelvic floor dysfunction
- Prescription medications such as oral contraceptives, acne medications, and hormonal suppressive therapies for diseases such as Endometriosis and Polycystic Ovarian Syndrome (PCOS)
- Surgical trauma (childbirth, pelvic organ prolapse repair, hysterectomy)
- Orthopedic injuries or traumas
- Biomechanical or structural dysfunction (hip dysfunction, sacro-iliac joint dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Vaginal childbirth
- Menopause
- Genital cutting or genital mutilation
Symptoms
- Repetitive vaginal and/or bladder infections and/or gynecologic, urologic, dermatologic or gastrointestinal conditions
- The majority of women with pelvic pain have pelvic floor dysfunction
- Prescription medications such as oral contraceptives, acne medications, and hormonal suppressive therapies for diseases such as Endometriosis and Polycystic Ovarian Syndrome (PCOS)
- Surgical trauma (childbirth, pelvic organ prolapse repair, hysterectomy)
- Orthopedic injuries or traumas
- Biomechanical or structural dysfunction (hip dysfunction, sacro-iliac joint dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Vaginal childbirth
- Menopause
- Genital cutting or genital mutilation

Diagnostic Challenges
Research shows that it can take up to five years for women with pelvic pain to get a proper diagnosis and up to 11 years for a woman with Endometriosis. This is because the symptoms of pelvic pain can mimic conditions such as urinary tract, yeast, bladder and sexually transmitted infections. When the pelvic floor is the culprit, the diagnostic tests for these infections are negative, leading to confusion for both the medical provider and the patient. Many medical providers are not aware that pelvic floor dysfunction can cause pelvic pain and it certainly does not occur to women to go to physical and occupational therapy when these symptoms arise. The majority of our patients tell us they did not know they even had a pelvic floor until things started to go wrong!
Diagnostic Challenges
Research shows that it can take up to five years for women with pelvic pain to get a proper diagnosis and up to 11 years for a woman with Endometriosis. This is because the symptoms of pelvic pain can mimic conditions such as urinary tract, yeast, bladder and sexually transmitted infections. When the pelvic floor is the culprit, the diagnostic tests for these infections are negative, leading to confusion for both the medical provider and the patient. Many medical providers are not aware that pelvic floor dysfunction can cause pelvic pain and it certainly does not occur to women to go to physical and occupational therapy when these symptoms arise. The majority of our patients tell us they did not know they even had a pelvic floor until things started to go wrong!
Treatment:
How We Can Help You

Women experiencing pelvic pain can benefit from an evaluation with a pelvic floor physical and occupational therapists specializing in pelvic pain. During the evaluation, the physical and occupational therapists reviews your history and symptoms with you, what you have been diagnosed with in the past, the treatments you have undergone and how effective or not effective these treatments have been. Importantly, we understand what you have been going through and that most women are frustrated by the time they get to see us. During the physical examination the physical and occupational therapists examines muscles, tissues, joints, nerves, and movement patterns. Once your physical and occupational therapists completes the examination they review your findings with you. The physical and occupational therapists creates an assessment which explains how you developed pain and creates short and long-term goals for your treatment plan. Typically, the frequency of physical and occupational therapy treatment is one to two times per week for roughly 12 weeks. You are given a home exercise program to compliment your in-person sessions, and your physical and occupational therapists will help to coordinate your recovery with the other members of your treatment team. We are here to help you recover and live your best life!

Treatment:
How We Can Help You
Women experiencing pelvic pain can benefit from an evaluation with a pelvic floor physical and occupational therapists specializing in pelvic pain. During the evaluation, the physical and occupational therapists reviews your history and symptoms with you, what you have been diagnosed with in the past, the treatments you have undergone and how effective or not effective these treatments have been. Importantly, we understand what you have been going through and that most women are frustrated by the time they get to see us. During the physical examination the physical and occupational therapists examines muscles, tissues, joints, nerves, and movement patterns. Once your physical and occupational therapists completes the examination they review your findings with you. The physical and occupational therapists creates an assessment which explains how you developed pain and creates short and long-term goals for your treatment plan. Typically, the frequency of physical and occupational therapy treatment is one to two times per week for roughly 12 weeks. You are given a home exercise program to compliment your in-person sessions, and your physical and occupational therapists will help to coordinate your recovery with the other members of your treatment team. We are here to help you recover and live your best life!
How Can We Help You?
Please use the form below to send us any questions or comments. You must include your e-mail address in order for us to send a response. Please be assured that all of your information will be kept confidential.

Join The Newsletter. Win a copy of our book, “Pelvic Pain Explained!”
We love getting to know our website visitors. Please tell us a little bit about yourself and get the latest info via PHRC e-newsletter!
*Subscribers automatically eligible to win our book, “Pelvic Pain Explained.”
At its heart, Pelvic Pain Explained is the story of how patients develop pelvic pain, the challenges patients and providers face throughout the diagnosis and treatment process, the difficult task of sifting through the different available treatment options, and the impact that an “invisible” condition has on a patient’s life and relationships, and much more.






 Jandra Mueller,DPT,MS
Jandra Mueller,DPT,MS